Why climate change is a global health crisis
Feature presented by the Global Climate and Health Alliance as part of the Climate and Us series.
Climate change is predicted to push an additional 132 million people into poverty worldwide by 2030 – of which one third will be caused by health factors. Increases in extreme weather events are also stretching healthcare services to their limits. How are countries preparing for more climate-related health crises?
When tropical storm Freddy arrived in Malawi in March 2023, it had already set records for its intensity and severity. While in Mozambique, the storm had previously been classified as a cyclone, which is stronger in intensity than a tropical storm, and reached wind speeds comparable to a Category 5 hurricane. The storm would eventually last for 36 days, making it one of the longest on record in the southern hemisphere. Climate change is increasing the intensity and duration of cyclones and storms, as warming seas fuel their strength (though there is some evidence that there will be fewer storms overall in the future).
But it was in Malawi where Freddy’s effects would be most significantly felt. The storm brought 600mm (24 inches) of rain in some areas, resulting in widespread flooding and landslides. Roads were washed away, houses flooded and lives destroyed. In total, more than 1,000 people died as a result of Freddy in Malawi. But healthcare professionals feared that the long-term effects of the storm might lead to many more deaths still.
“With Malawi already having a very lengthy and aggressive cholera outbreak, and then experiencing Freddy on top of that, we were anticipating that we would have very high cases of cholera,” says Anda Nindi Nyondo, country director for Malawi at Seed Global Health, a non-profit organisation who have been training family medicine physicians and midwives in Malawi for more than a decade, among other sub-Saharan countries.
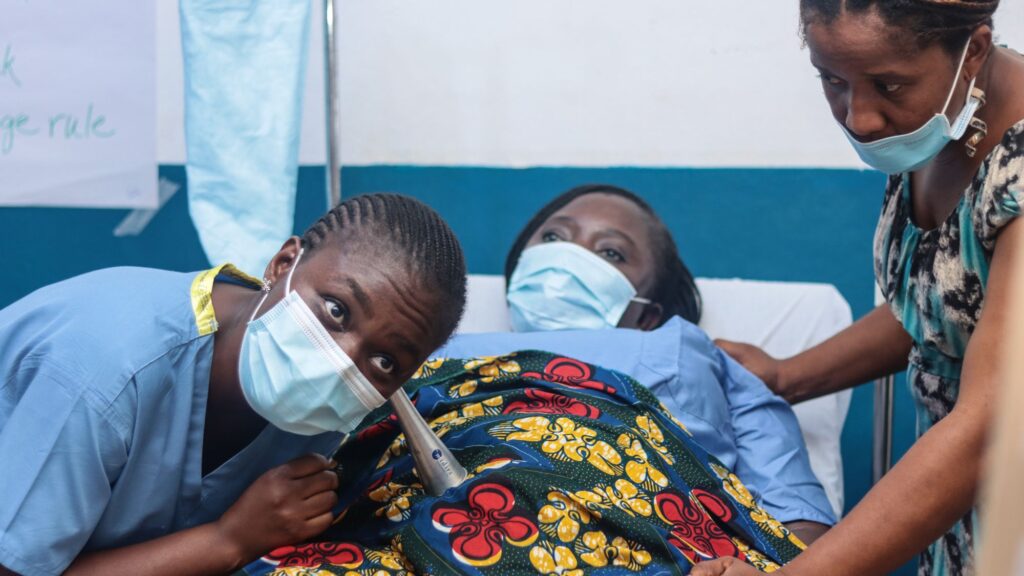
Healthcare workers carrying out checks
Tens of thousands of cases of cholera had already been reported in Malawi before Freddy arrived. The outbreak started around February 2022 after tropical storm Ana arrived in January. These months are typically Malawi’s rainy season, and with cholera being endemic in the country, Nyondo says healthcare experts expect that each rainy season will bring more cases.
People who live on the shores of Lake Malawi are particularly at risk of the effects of flooding. “And these people were being housed in temporary camps where sanitation is always questionable and safe water sources are very, very scarce,” says Nyondo. “So that means poor water sources, poor sanitation and poor latrines – especially for people who have to go very far to get clean water. Those people use the streams and rainwater sources which are nearer during the rainy season. So this would make them more likely to get cholera.”
“Climate change impacts us in such myriad ways,” says Vanessa Kerry, a physician, CEO and co-founder of Seed Global Health and the World Health Organization’s director-general special envoy for climate change and health. “It’s direct trauma, it’s loss of housing, it’s changes in food and agriculture, it’s changes in water security. It is also then the direct health impacts in terms of non-communicable diseases, communicable diseases, mental health, maternal health.”
But something unusual happened after Freddy. Despite the high number of cholera cases, and the undoubted devastation that the storm brought, the new cholera cases weren’t as high as Nyondo and others had anticipated. “The numbers did increase, but not to the alarming state that we thought.”

“We [Malawi] had strategies in place already that ended up helping to contain the cholera cases,” adds Nyondo. “We had people already in the districts in place to work on the water and sanitation. There were already treatment camps and facilities to be able to screen and diagnose or disease surveillance. So it was easier to respond.”
We spend a lot more time, energy and resources responding to crises – Vanessa Kerry
During emergencies, Nyondo says that the districts they work with are set up to make rapid assessments of their priorities. By having a flexible trained workforce at the ready, non-communicable diseases, mental health burdens, maternal mortality, and infectious diseases can be treated rapidly. Some of these rapid responses are based on lessons from Covid-19.
“I think what people don’t realise is we spend a lot more time, energy and resources responding to crises,” says Kerry. A better approach, she adds, is to prepare well for crises.
Preparation is key
The earliest origins of Seed Global Health started when Kerry was 14 in Vietnam. She saw poverty and a lack of resources that she says she had never seen before. “I’m not going to say I knew what to do with it at that moment, but I definitely carried it with me such that when I went into my medical career, I knew I needed to incorporate that experience into the work I did. It influenced where I chose to go to medical school. I then had a series of opportunities where I worked in Uganda, Rwanda and Ghana, and that reinforced the fact that there are two very different standards of healthcare in the world.”
But, she adds, disparities in access to and quality of healthcare are seen in countries all over the world, including the US, UK and other more developed nations.

To date, Seed Global Health has trained 34,000 doctors, nurses and midwives in seven countries in Sub-Saharan Africa. “And, we’re supporting building an emergency medicine system in Uganda where over half the deaths are from a failure of emergency and triage services,” says Kerry. “We’re building up family medicine in Zambia where at least 70% of the healthcare problems, be it from climate change or generally, can be treated by a general GP-like physician. We started Seed with a deep belief that people are the backbone of strong health systems.”
We’re not going to escape the impacts of climate change – we’re living it – Vanessa Kerry
Seed Global Health’s investment in human resources is something that inspires Nyondo. “We will begin training healthcare providers to not think about climate change and health separately, but to automatically and deliberately think about them as linked,” she says.
Kerry reiterates that the impact of climate change on health is not a future problem, but one that we are experiencing now considering that, for example, 6.7 million people die each year from air pollution. “We’re talking about our survival here,” says Kerry. “I think that’s what folks need to begin to understand – we’re not going to escape the impacts of climate change because we’re living it. I think there’s a win-win path forward [by improving healthcare and mitigating climate change], but it’s about helping people to understand what that is.”

Kerry and Nyondo reiterate that there is a long way to go. Kerry cites women dying daily in Sierra Leone from postpartum haemorrhage as one example of why the work of Seed and partners is so critical.
“The decisions we’ve been making collectively as a society I would consider to be a pandemic of poor and expedient choices – short-term wins,” says Kerry. “We can’t work that way anymore. At this moment in time we are at one of the most existential and tumultuous times in modern history. And I think we have to ask ourselves what is a way forward?”